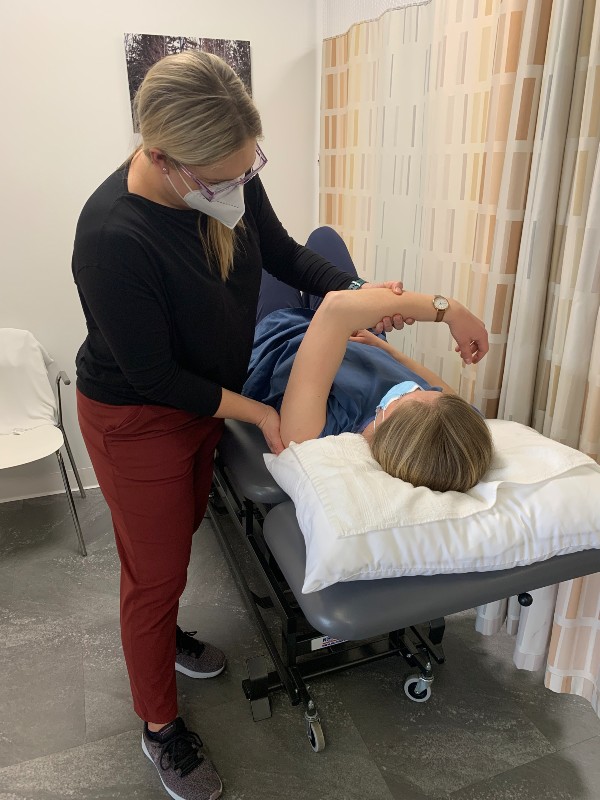
By far, the 2 most common conditions we see at our Clinic is low back pain followed closely by shoulder pain. For our March blog, Danielle Bles discusses a common condition that affects shoulders called Frozen Shoulder. What is it and what can be done to treat this painful condition? Read on!
Frozen shoulder or Adhesive Capsulitis is a very painful condition that affects 2-5% of the population, most commonly between the ages of 40 and 60 (1,2,4). Often there is no preceding injury; it can happen insidiously or without any inciting event. Most begin with a persistent pain that steadily progresses into significant stiffness and reduced shoulder function.
The condition tends to progress through 3 phases although not always in a linear fashion. In total these can last from approximately 6 months to 2 or more years.
Phase 1: The acute/painful phase
- typically begins with an ache that progressively worsens.
- night pain is common but there is no significant stiffness in the shoulder in this phase
Phase 2: The stiffening/freezing/adhesive phase
- progressive stiffening of the shoulder joint along with severe pain. Typically there is a loss of the ability to reach behind the back, out to the side and overhead.
Phase 3: The resolution/thawing phase
- Gradual improvement of pain symptoms as well as range of motion of the shoulder joint. Many people proceed to full resolution of symptoms.
How is it diagnosed?
A frozen shoulder has a very specific pattern of stiffness which is characterized by a loss of external rotation, abduction and internal rotation (3). The shoulder demonstrates stiffness with both active (moving with your own force) and passive (moving with assistance) movements (1,2,3,4) . A physician or physiotherapist can diagnose a frozen shoulder based on your clinical examination. Shoulder osteoarthritis can also mimic a frozen shoulder so a simple x-ray can rule out arthritis or other joint pathology if this is suspected. X-rays in a frozen shoulder are usually normal (3).
What are the treatment options?
- Physiotherapy
Physiotherapy has been shown to be effective in treating many cases of adhesive capsulitis (4). Manual therapy, muscle release techniques and dry needling are all useful modalities to improve your pain and mobility. A home exercise program that is personalized to your specific findings and restrictions is an important part of your management. In many cases the combination of time and physiotherapy is enough to progressively resolve symptoms.
- Injections
There have been many studies evaluating various injections as a treatment option (1,2,3,4). The two most common are intra-articular cortisone injections (an injection into the joint) and hydrodilatation which is a combination of an intra-articular cortisone injection along with saline in an attempt to stretch and expand the joint capsule from the inside (1,2,3,4). Many studies have documented significant pain relief and improvement of movement with both of these injections (1,2,3). The addition of physiotherapy and a good home program tend to improve the outcomes of injections versus injections alone (3). - Surgery
In the most resistant cases where physiotherapy and injections have not been effective in restoring shoulder function, surgery may be warranted (1). The surgery consists of a manipulation of the shoulder under anaesthesia with or without a capsular release procedure (1). Most cases of frozen shoulders do not require surgical intervention.

It is important to note that presentations can vary considerably between two people with the same diagnosis. Some people only get a mild version that resolves within 6 months with minimal effect on their quality of life. Some people lose significant range of motion where basic activities of daily living such as dressing and washing their hair are difficult and their pain at night is considerable. As always, just as in other injuries and conditions, the choice of treatment will depend on a person’s presentation and their progress. Physiotherapy and a good home program should always be tried first with the decision to proceed with injections only as a second option if a person’s progress is either too slow or the condition is too painful.
Cookie cutter approaches do not work. A personalized assessment and treatment program is essential!
References
- Catapano, M., et al. Hydrodilatation With Corticosteroid for the Treatment of Adhesive Capsulitis: A Systematic Review. PM&R 2018 10:623-635.
- Hashmi, M.U., Chugtai, B.B., & Ahsan, M.N. Adhesive Capsulitis: Management by Physiotherapy Versus Intra-articular Corticosteroid Injection. Pak Armed Forces Med 2021, 71(5): 1824-1827.
- Singh, P., et al. Hydrodilatation: The Effective Treatment Modality in Adhesive Capsulitis. Journal of Orthopedics, Traumatology and Rehabilitation 2019 11: 100-103.
- Sun, Y., et al. Steroid injection Versus Physiotherapy for Patients With Adhesive Capsulitis of the Shoulder. Medicine 2016. 95(20): 1-9.
Submitted by Danielle Bles.
